They provide an intensive rehabilitation program and patients who are admitted must be able to tolerate three hours of intense rehabilitation services per day. CMS collects patient assessment data only on Medicare Part A fee-for service patients.
What does Medicare Part a cover for rehab?
Dec 01, 2021 · Rehabilitation Agency - An agency that provides an integrated, multidisciplinary program designed to upgrade the physical functions of handicapped, disabled individuals by bringing together, as a team, specialized rehabilitation personnel. Clinic- A facility established primarily for the provision of outpatient physicians’ services. To meet the definition of a clinic, …
What are the Medicare guidelines for inpatient rehabilitation?
Medicaid Services (CMS) published a final rule that revised §412.23(b)(2). Under revised §412.23(b)(2), a specific compliance percentage threshold of an IRF’s total patient population must require intensive rehabilitation services for the treatment of one or more of the specified conditions. Based on the final rule, CMS issued a Joint
How much does Medicare pay for inpatient rehab?
Feb 15, 2022 · Learn more about Section 3004 of the ACA (Quality Reporting for Long-Term Care Hospitals (LTCH), Inpatient Rehabilitation Facilities (IRF), and Hospice Programs) by visiting P.L. Public Law No: 111-148 (H.R. 3590 Health Care Law). The Improving Medicare Post-Acute Care Transformation (IMPACT) Act of 2014 added Section 1899B to the SSA, which ...
How long will Medicare cover rehab in a skilled nursing facility?
Inpatient rehabilitation care. Part A covers inpatient hospital stays, care in a skilled nursing facility, hospice care, and some home health care. Health care services or supplies needed to diagnose or treat an illness, injury, condition, disease, or its symptoms and that meet accepted standards of medicine.

What are some CMS criteria for inpatient rehabilitation facilities?
Recently, the Centers for Medicare & Medicaid Services (CMS) advised its medical review contractors that when the current industry standard of providing in general at least 3 hours of therapy (physical therapy, occupational therapy, speech-language pathology, or prosthetics/orthotics) per day at least 5 days per week ...Dec 20, 2018
What are the levels of rehab?
Read on for our rundown of the eight most common rehab settings.Acute Care Rehab Setting. ... Subacute Care Rehab Setting. ... Long-term Acute Care Rehab Setting. ... Home Health Care Rehab Setting. ... Inpatient Care Rehab Setting. ... Outpatient Care Rehab Setting. ... School-Based Rehab Setting. ... Skilled Nursing Facility Rehab Setting.
What are the CMS 13 diagnosis?
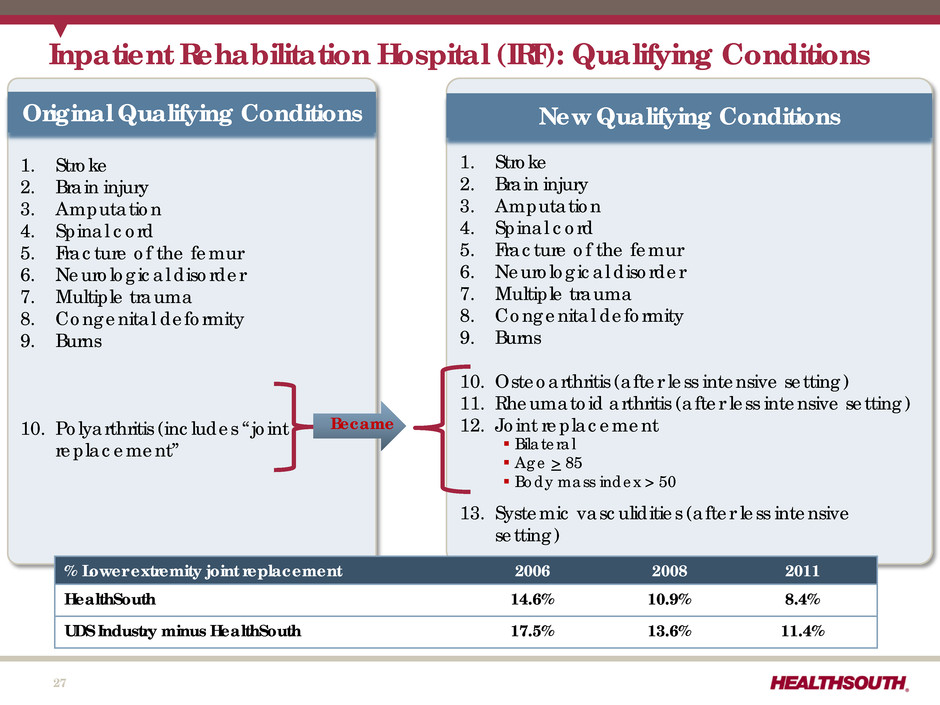
Understanding qualifying conditions for admissionStroke.Spinal cord injury.Congenital deformity.Amputation.Major multiple trauma.Fracture of femur.Brain injury.Neurological disorders.More items...
What is a rehab impairment category?
Represent the primary cause of the rehabilitation stay. They are clinically homogeneous groupings that are then subdivided into Case Mix Groups (CMGs).
What are the 3 types of rehab?
The three main types of rehabilitation therapy are occupational, physical and speech. Each form of rehabilitation serves a unique purpose in helping a person reach full recovery, but all share the ultimate goal of helping the patient return to a healthy and active lifestyle.May 23, 2018
What are the 4 types of rehabilitation?
Rehabilitation ElementsPreventative Rehabilitation.Restorative Rehabilitation.Supportive Rehabilitation.Palliative Rehabilitation.
When Medicare runs out what happens?
Medicare will stop paying for your inpatient-related hospital costs (such as room and board) if you run out of days during your benefit period. To be eligible for a new benefit period, and additional days of inpatient coverage, you must remain out of the hospital or SNF for 60 days in a row.
What is a rehab diagnosis?
The main difference is that in rehabilitation the presenting problems are limitations in activities and the main items investigated are impairment and contextual matters, whereas in medicine the presenting problems are symptoms, and the goals are the diagnosis and treatment of the underlying disease.
What is a hospital DPU?
Certain institutions may qualify a part of their hospital for exclusion from the Prospective Payment System (PPS) as Distinct Part Units (DPU). Psychiatric, Rehabilitation, Children's, Long-Term Care Units (LTACH), Skilled Nursing Facilities (SNF) and Cancer Hospitals, are eligible to qualify for the exclusion.Mar 19, 2021
What are the 3 contributing factors that determine the level of E M service?
To bill any code, the services furnished must meet the definition of the code. You must ensure that the codes selected reflect the services furnished. The three key components when selecting the appropriate level of E/M services provided are history, examination, and medical decision making.
What is the labor portion of the IPF PPS?
70.317 percentWhat is the labor portion of the IPF PPS per diem rate? What is the non-labor portion of the IPF PPS per diem rate? 70.317 percent is the labor portion and 29.683 percent is the non-labor portion.
Which tool is administered to all patients admitted to an inpatient rehabilitation facility?
1 An Inpatient Rehabilitation Facility Patient Assessment Instrument (IRF PAI) is used to collect data that drives payment. It must be completed on admission and upon discharge of the patient from the IRF.
What is section 3004?
Section 3004 of the Affordable Care Act. CMS has created a website to support Section 3004 of the Affordable Care Act, Quality Reporting for Long Term Care Hospitals, Inpatient Rehabilitation Hospitals and Hospice Programs.
What is IRF PPS?
Historically, each rule or update notice issued under the annual Inpatient Rehabilitation Facility (IRF) prospective payment system (PPS) rulemaking cycle included a detailed reiteration of the various legislative provisions that have affected the IRF PPS over the years. This document (PDF) now serves to provide that discussion and will be updated when we find it necessary.
When is the new U07.1 code?
The new code, U07.1, can be used for assessments with a discharge date of April 1, 2020 and beyond. Section 4421 of the Balanced Budget Act of 1997 (Public Law 105-33), as amended by section 125 of the Medicare, Medicaid, and SCHIP (State Children's Health Insurance Program) Balanced Budget Refinement Act of 1999 (Public Law 106-113), ...
What is a rehabilitation agency?
Rehabilitation Agency - An agency that provides an integrated, multidisciplinary program designed to upgrade the physical functions of handicapped, disabled individuals by bringing together, as a team, specialized rehabilitation personnel.
What is a clinic?
Clinic - A facility established primarily for the provision of outpatient physicians’ services. To meet the definition of a clinic, the facility must meet the following test of physician participation:#N#The medical services of the clinic are provided by a group of three or more physicians practicing medicine together; and#N#A physician is present in the clinic at all times during hours of operation to perform medical services (rather than only administrative services). 1 The medical services of the clinic are provided by a group of three or more physicians practicing medicine together; and 2 A physician is present in the clinic at all times during hours of operation to perform medical services (rather than only administrative services).
What is Medicare certified hospital?
Section 1886(d)(1)(B) of the Social Security Act (the Act) and Part 412 of the Medicare regulations define a Medicare certified hospital that is paid under the inpatient (acute care hospital) prospective payment system (IPPS). However, the statute and regulations also provide for the classification of special types of Medicare certified hospitals that are excluded from payment under the IPPS. These special types of hospitals must meet the criteria specified at subpart B of Part 412 of the Medicare regulations. Failure to meet any of these criteria results in the termination of the special classification, and the facility reverts to an acute care inpatient hospital or unit that is paid under the IPPS in accordance with all applicable Medicare certification and State licensing requirements. In general, however, under §§ 412.23(i) and 412.25(c), changes to the classification status of an excluded hospital or unit of a hospital are made only at the beginning of a cost reporting period.
When was the CMS rule for major multiple traumas?
In the proposed rule dated September 9, 2003 (FR 68, 53272) CMS clarified which patients should be counted in the category of major multiple traumas to include patients in diagnosis-related groups 484, 485, 486 or 487 used under the IPPS.
What is Medicare IRF?
All hospitals or units of a hospital that are classified under subpart B of part 412 of the Medicare regulations as inpatient rehabilitation facilities (IRFs). Medicare payments to IRFs are based on the IRF prospective payment system (PPS) under subpart P of part 412.
What is 412.23(b)(2)?
Under revised §412.23(b)(2), a specific compliance percentage threshold of an IRF’s total patient population must require intensive rehabilitation services for the treatment of one or more of the specified conditions. Based on the final rule, CMS issued a Joint Signature Memorandum including instructions related to Regional Office (RO) and Medicare fiscal intermediary (FI) responsibilities regarding the performance of reviews to verify compliance with §412.23(b)(2) as detailed in CRs 3334 and 3503, which revised Medicare Claims Processing Manual Chapter 3, sections 140.1 to 140.1.8. (CR 3503 corrected some errors or clarified the instructions in CR 3334 and presented additional instructions to implement revised §412.23(b)(2).
When was the 412.23(b)(2) review suspended?
On June 7 , 2002, CMS notified all ROs and FIs of its concerns regarding the effectiveness and consistency of the review to determine compliance with §412.23(b)(2). As a result of these concerns, CMS initiated a comprehensive assessment of the procedures used by the FIs to verify compliance with the compliance percentage threshold requirement and suspended enforcement of the compliance percentage threshold requirement for existing IRFs. The suspension of enforcement did not apply to a facility that was first seeking classification as an IRF in accordance with §412.23(b)(8) or §412.30(b)(2). In such cases, all current regulations and procedures, including §412.23(b)(2), continued to be required.
What is IRF QRP?
What is the IRF QRP? The IRF QRP creates IRF quality reporting requirements, as mandated by Section 3004 (b) of the Patient Protection and Affordable Care Act (ACA) of 2010.
What is the impact act?
The Improving Medicare Post-Acute Care Transformation (IMPACT) Act of 2014 added Section 1899B to the SSA, which requires the reporting of standardized patient assessment data about quality measures and Standardized Patient Assessment Data Elements (SPADEs).
What is part A in rehabilitation?
Inpatient rehabilitation care. Part A covers inpatient hospital stays, care in a skilled nursing facility, hospice care, and some home health care. Health care services or supplies needed to diagnose or treat an illness, injury, condition, disease, or its symptoms and that meet accepted standards of medicine.
How long does it take to get into an inpatient rehab facility?
You’re admitted to an inpatient rehabilitation facility within 60 days of being discharged from a hospital.
What is the benefit period for Medicare?
benefit period. The way that Original Medicare measures your use of hospital and skilled nursing facility (SNF) services. A benefit period begins the day you're admitted as an inpatient in a hospital or SNF. The benefit period ends when you haven't gotten any inpatient hospital care (or skilled care in a SNF) for 60 days in a row.
Does Medicare cover private duty nursing?
Medicare doesn’t cover: Private duty nursing. A phone or television in your room. Personal items, like toothpaste, socks, or razors (except when a hospital provides them as part of your hospital admission pack). A private room, unless medically necessary.
Does Medicare cover outpatient care?
Medicare Part B (Medical Insurance) Part B covers certain doctors' services, outpatient care, medical supplies, and preventive services.
Where does rehabilitation take place?
Rehabilitation may take place in a special section of the hospital, in a skilled nursing facility, or in a separate rehabilitation facility. Although Medicare covers your care during rehabilitation, it’s not intended to be long-term care. You can learn more about Medicare and long-term care facilities here.
What to do if you have a sudden illness?
Though you don’t always have advance notice with a sudden illness or injury, it’s always a good idea to talk with your healthcare team about Medicare coverage before a procedure or inpatient stay, if you can.
Does Medicare cover rehab?
Medicare Part A covers your inpatient care in a rehabilitation facility as long as your doctor deems it medically necessary. In addition, you must receive care in a facility that’s Medicare-approved. Depending on where you receive your inpatient rehab therapy, you may need to have a qualifying 3-day hospital stay before your rehab admission.
Does Medigap cover coinsurance?
Costs with Medigap. Adding Medigap (Medicare supplement) coverage could help you pay your coinsurance and deductible costs. Some Medigap plans also offer additional lifetime reserve days (up to 365 extra days). You can search for plans in your area and compare coverage using Medicare’s plan finder tool.
Does Medicare cover knee replacement surgery?
The 3-day rule does not apply for these procedures, and Medicare will cover your inpatient rehabilitation after the surgery. These procedures can be found on Medicare’s inpatient only list. In 2018, Medicare removed total knee replacements from the inpatient only list.
Does Medicare cover inpatient rehabilitation?
Medicare covers your treatment in an inpatient rehabilitation facility as long as you meet certain guidelines.
How long does Medicare cover SNF?
After day 100 of an inpatient SNF stay, you are responsible for all costs. Medicare Part A will also cover 90 days of inpatient hospital rehab with some coinsurance costs after you meet your Part A deductible. Beginning on day 91, you will begin to tap into your “lifetime reserve days.".
How much is Medicare Part A deductible for 2021?
In 2021, the Medicare Part A deductible is $1,484 per benefit period. A benefit period begins the day you are admitted to the hospital. Once you have reached the deductible, Medicare will then cover your stay in full for the first 60 days. You could potentially experience more than one benefit period in a year.
Who is Christian Worstell?
Christian Worstell is a licensed insurance agent and a Senior Staff Writer for MedicareAdvantage.com. He is passionate about helping people navigate the complexities of Medicare and understand their coverage options. .. Read full bio
Does Medicare cover outpatient treatment?
Medicare Part B may cover outpatient treatment services as part of a partial hospitalization program (PHP), if your doctor certifies that you need at least 20 hours of therapeutic services per week.
Is Medicare Advantage the same as Original Medicare?
Medicare Advantage plans are required to provide the same benefits as Original Medicare. Many of these privately sold plans may also offer additional benefits not covered by Original Medicare, such as prescription drug coverage.
Does Medicare cover rehab?
Learn how inpatient and outpatient rehab and therapy can be covered by Medicare. Medicare Part A (inpatient hospital insurance) and Part B (medical insurance) may both cover certain rehabilitation services in different ways.